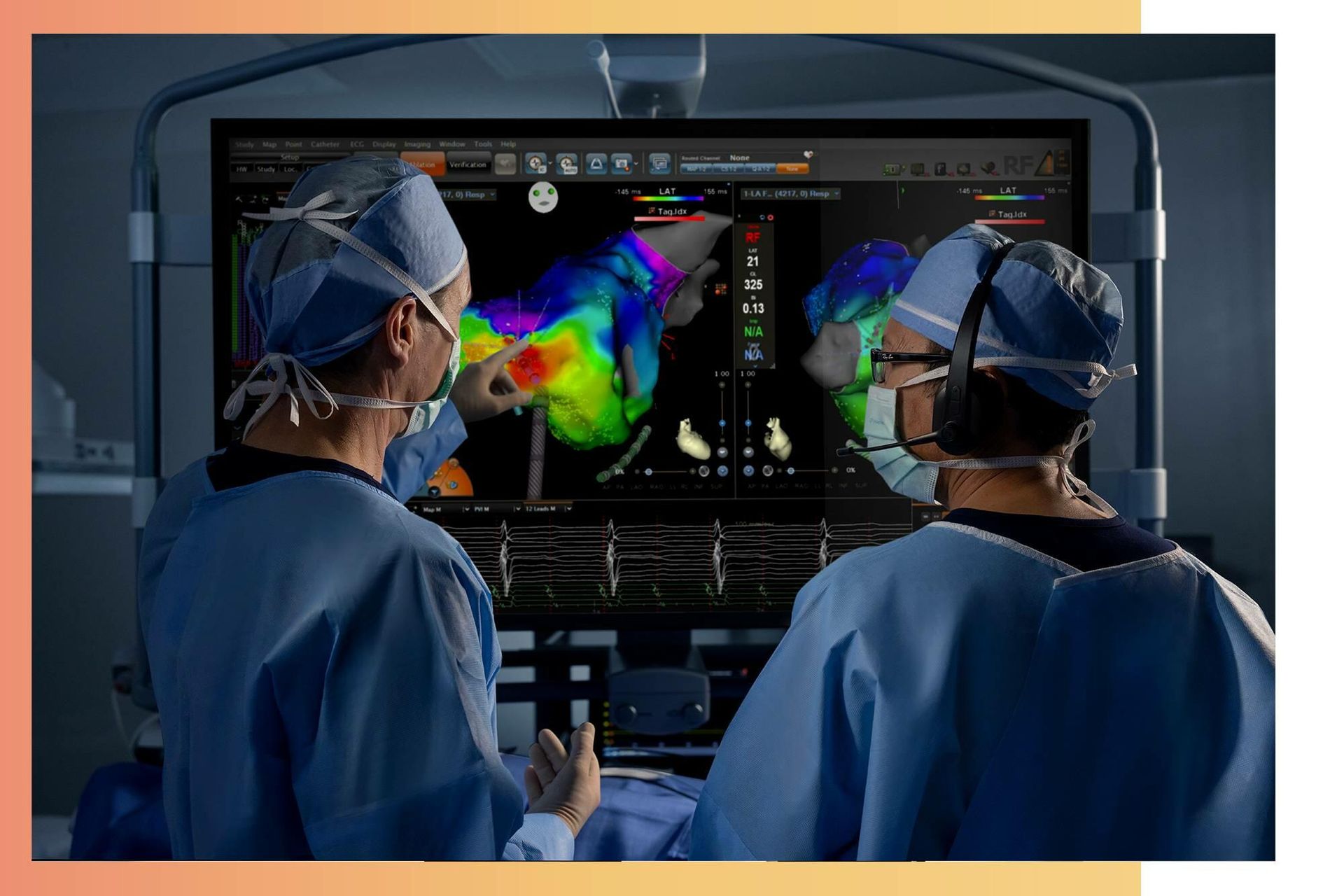
Innovative Technologies Shaping the Future of Rural Healthcare
As an experts in international medical recruitment, we note that rural and remote medical practice has generated increased demand for general practitioners, specialists in permanent and locum jobs and junior doctors seeking vocational training in this growing field. We are intrigued by developments in this sector. Today, we share some information about the cutting-edge technologies, from drones to wearables to Artificial Intelligence which are revolutionising healthcare and altering the access and delivery of healthcare in rural areas.
People living in regional and rural areas face unique challenges due to their geographical location and often have poorer health outcomes than people living in metropolitan areas, with higher rates of hospitalisations, deaths, injury, and poorer access to primary health services. Rural and remote areas have an estimated double the number of preventable hospitalisations and potentially avoidable deaths compared to metropolitan areas.
In Australia, around 7.3 million people or 28% of the population live in rural and remote regions and 32% of this demographic is Fist Nations Australians. According to the Australian Institute of Health and Welfare and the National Indigenous Australians Agency, First Nations Australians have lower life expectancies, a high burden of disease, poorer self-reported health and a higher likelihood of being hospitalised than non-Indigenous Australians. In Canada, the world's second largest country, 16% of the population live in rural areas.
It is no surprise that Australia leads the world in many important initiatives to address rural healthcare inequalities including the creation of Rural and Remote Medicine as a speciality and the development of new technologies, especially drones.
The Rise of Drones in Healthcare
Unmanned Aircraft Systems named drones, once reserved only for military use, are now making a significant impact in healthcare by delivering lifesaving drugs, medical equipment, and supplies, thus providing immediate and vital assistance when and where it is needed most. Current drone technology is often limited by distance capacity but Australia has a plan to create a hydrogen-fuelled carbon-neutral VTOL UAV that can carry medical cargo, while providing unparalleled range.
The Wildu Aero Project Australia
One of the world's first medical drone projects is the Wildu Aero Project led by Associate Professor Dries Verstraete from the University of Sydney. A Dutch engineer, Dries, has developed a hydrogen-fueled, emissions free medical drone able to travel large distances, in partnership with ASAC Consultancy, a consultancy firm dedicated to bridging the gap in health inequalities, which has funded research and development for a hydrogen fuelled vertical take-off and landing (eVTOL) uncrewed aerial vehicle (UAV).
The medical drone is being designed to enable early detection, prevention, and treatment of health conditions common in rural and remote regions of Australia, such as sepsis, and to actively contribute to addressing the health inequities for some of Australia’s most vulnerable and isolated communities.
The Wildu Aero Project will complement local primary health networks, telehealth services, pathology services and pharmaceutical delivery. It will enable the use of other innovative technologies and support the function of emergency and disaster management operations, such as during infection outbreaks or when communities are cut off by floods.
Benefits of Telemedicine in Rural Healthcare
Telemedicine is widely used in rural medicine for remote consultations between doctors and patients and also increasingly between rural doctors and urban hospital specialists for real time advice on patient management. It uses video conferencing technologies to facilitate contact and has made a tremendous impact on rural medicine by improving access to preventative and curative healthcare and reducing the need for long distance travel. benefits include:
Improved Access to Healthcare Services
Remote consultations enable rural patients to consult specialists without the need for long-distance travel to urban hospitals which is especially important in areas where specialists are scarce or located far away. Virtual consultations allow for quicker responses to health concerns, preventing delays in diagnosis or treatment. Doctors can easily monitor and manage patients remotely, reducing waiting times for appointments. Telemedicine is especially useful to expand access to counseling and psychiatric care, which is crucial for communities that may otherwise struggle with mental health service availability.
Enhanced Continuity of Care
Telemedicine allows doctors to follow up with patients who suffer from chronic conditions (e.g., diabetes, hypertension) through remote monitoring devices. This ensures regular check-ups, medication adherence, and timely adjustments to treatment plans without requiring patients to travel long distances.
Reduction in Travel Time and Costs for Patients
For patients in remote rural areas, traveling to see a healthcare provider can be time-consuming and expensive. Telemedicine reduces the need for long journeys, lowering transportation costs and making healthcare more accessible. Patients can have virtual consultations from the comfort of their homes, improving their overall healthcare experience. This convenience can lead to better patient satisfaction and greater engagement in their own care.
Addressing Healthcare Workforce Shortages
Rural areas often struggle with a lack of medical specialists. Telemedicine helps bridge this gap by allowing rural doctors to consult with specialists virtually, ensuring that patients receive expert opinions and comprehensive care. It also fosters collaborative care models, where rural healthcare providers can easily consult with urban hospitals or medical centers, improving the quality of care in isolated areas. By enabling doctors to manage routine consultations remotely, telemedicine can help reduce the workload in rural clinics, preventing burnout and promoting better work-life balance for physicians.
Cost-Effective Healthcare Delivery
Telemedicine is more cost-effective than traditional in-person visits and reduces the overall costs of healthcare provision. It eliminates the need for physical office space, travel costs, and administrative overhead associated with in-person appointments. By offering regular remote check-ups and monitoring, telemedicine can help prevent complications and hospitalizations, ultimately saving costs for both patients and healthcare systems. Early detection through virtual visits can prevent the need for more expensive treatments later.
Flexibility and Convenience for Healthcare Providers
Doctors can expand their practice to a broader geographic area, reaching underserved populations without the need for a physical presence. This is particularly beneficial for specialists who are often in high demand. Virtual consultations can be scheduled more flexibly, allowing healthcare providers to manage their time better, avoid long waiting times, and optimize their day by balancing in-person and virtual appointments. Doctors can use telemedicine for routine check-ups or non-urgent cases (e.g., prescription refills, minor health concerns), enabling more face-to-face time for complex or emergency cases.
The Role of AI in Rural Healthcare
Artificial Intelligence (AI) is creating a silent revolution in rural health in which lies an unprecedented opportunity for the international development sector to break down the walls of disparity and deliver hope to communities long overlooked by modern medicine. There are five transformative AI opportunities which can redefine the very fabric of rural health.
1. AI-Powered Telemedicine Platforms
Low-bandwidth, AI-powered telemedicine platforms which can operate effectively in rural areas with limited connectivity can be designed to be accessible via basic smartphones and feature simplified user interfaces for both patients and healthcare providers. These facilitate seamless remote consultations and referrals, ensuring no community is left behind in accessing essential medical services.
2. Mobile Health Applications
AI-driven mobile health applications, like M-Tiba in Kenya can provide comprehensive healthcare services, from maternal and child health to chronic disease management, empowering rural populations to take control of their health through personalised and accessible digital solutions. These can be designed to work offline and feature interactive educational content, symptom checkers, and appointment scheduling functionalities.
3. Predictive Analytics and Diagnostics
AI-powered predictive analytics and diagnostics solutions such as the TB Detection Tool in India, can be used for disease prediction and early detection in resource-limited settings. The seamless integration of predictive analytics into existing healthcare frameworks, contributing to long-term sustainability.
4. Remote Monitoring and Wearable Devices
AI-driven remote monitoring and wearable devices, similar to the Pumani CPAP machine in Malawi are a valuable tool for improving healthcare in rural areas by providing real-time health data to doctors and patients. Remote monitoring devices can track vital signs like heart rate, blood pressure, and glucose levels, providing objective health data which allows doctors to monitor patients remotely and make clinical decisions. Their use has lead to improved clinical outcomes and reduced hospital readmissions proving their use as a cost-effective way to provide healthcare in rural areas.
5. Healthcare Robotics and Automation
AI-driven robotics and automation solutions like the Smart Glasses for Cataract Surgery in Nepal, are cost-effective robotic-assisted surgical systems which can be deployed in rural areas by training local healthcare workers on robotic-assisted procedures.
For rural healthcare, AI has transformative potential, offering remote patient monitoring and telehealth services, thus bridging the gap between limited healthcare access and the need for timely, critical care.
As telemedicine, artificial intelligence and drone technology continues to transform healthcare delivery in rural areas, there has never been a better time for doctors to explore opportunities in rural medical practice. Not only can you make a significant impact by bringing quality healthcare to underserved communities, but you can also benefit from the flexibility, professional growth, and technological advancements that these technologies offer.
Take action today:
- Register for jobs in rural medical practice and become a part of the innovative future of healthcare.
- Help bridge the healthcare gap by bringing much-needed services to areas where specialists and healthcare providers are in short supply.
- Experience the fulfillment of making a difference while enjoying the benefits of telemedicine, including flexible work hours and the ability to manage patient care remotely.
Join the growing number of healthcare professionals who are leading the way in rural healthcare innovation. Register today and start your journey toward a rewarding career that makes an immediate impact.
22 November 2024
Share this post on Social Media