A Comprehensive Guide to Radiology and Associated Subspecialities
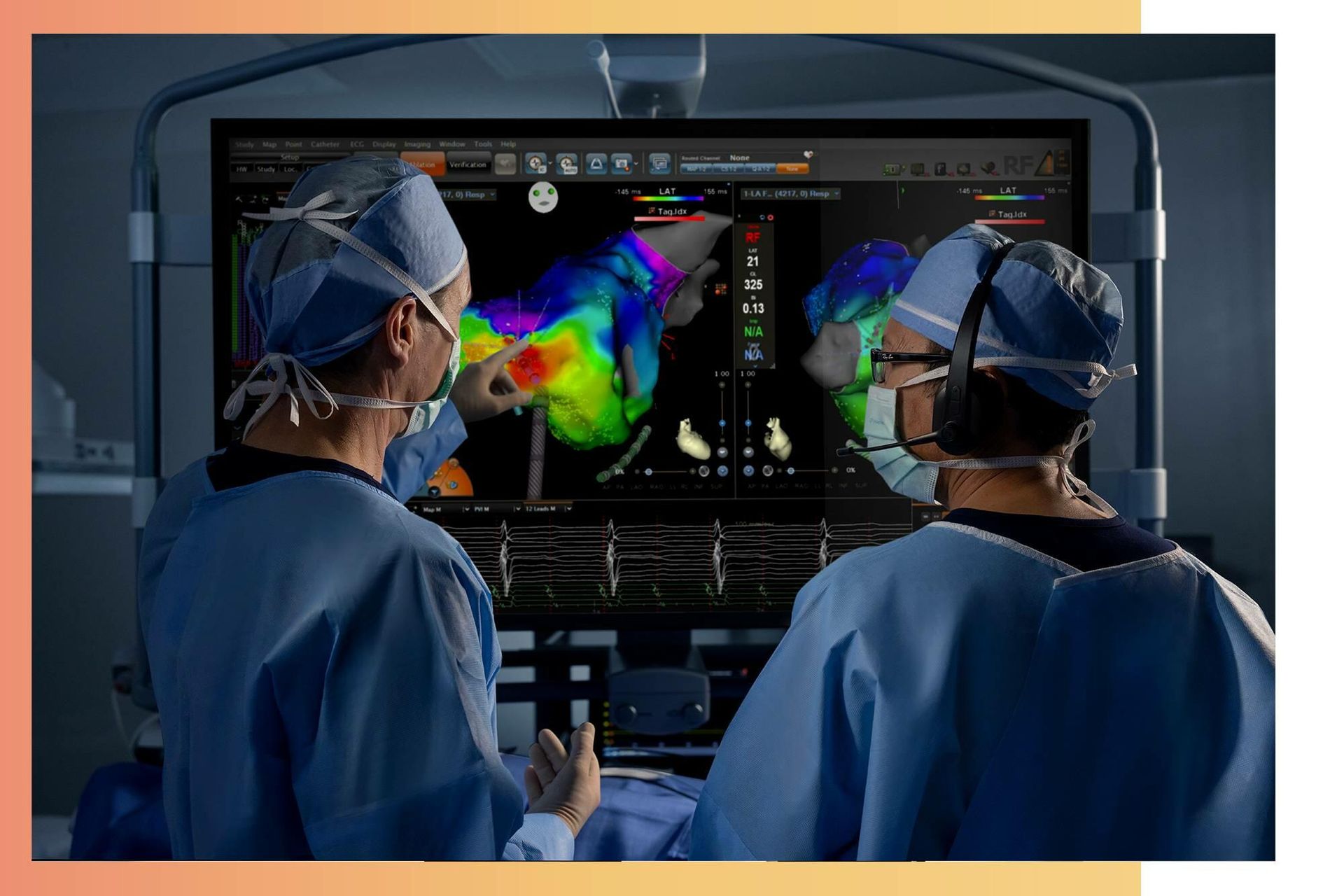
Radiology is an indispensable part of patient care, critically intersecting with all areas of clinical medicine by enhancing diagnostic accuracy and providing the means for minimally invasive interventional procedures. Its growth from a marginal speciality to one of medicine's fastest growing is attributable to the technological innovation which has powered the development of new imaging modalities and subspecialist fields.
In this article, we have compiled a comprehensive guide to provide an in-depth overview of radiology subspecialties.
The Scope of Radiology Subspecialties
Initially limited to the interpretation of plain Xray patient examinations, radiology has swiftly developed in recent years to become one of medicine's fastest growing and exciting fields. This explosive transformation was brought about by new technologies adapted to enhance medical imaging capabilities, leading to improved diagnostic capacity and the potential for interventional procedures as an adjunct to or replacement for open surgical operations.
The five major modalities of radiology, namely, X Ray, Computerised Tomography (CT), Magnetic Resonance Imaging (MRI), ultrasound and Positron emission tomography (PET) have driven the growth of the speciality and its diversification into a growing range of subspecialist fields.
Diagnostic Radiology
Diagnostic Radiology remains the principal scope of practice for most radiologists worldwide who practise in this field exclusively or in combination with a subspecialist interest. Working in a variety of clinical facilities, from rural to metropolitan hospitals, the typical practice is varied and requires a broad range of experience.
Tele-radiology whereby radiological images, such as CT scans and X-Rays, are transmitted and displayed in a location independent of the location where the patient is imaged, is gaining popularity to allow radiologists to provide expert reports quickly. Images may be sent across organisational and even national borders. This provides an alternative practice model to hospital based radiology and new career opportunities.
Interventional Radiology
Interventional radiology(IR) is the only officially recognised sub-specialty of clinical radiology for the purposes of most professional regulatory authorities, although there is a breadth of other subspecialist areas to be studied.
Interventional radiologists use image-guided procedures to diagnose and treat diseases. IR procedures are minimally invasive, often requiring smaller incisions than traditional surgery. Interventional Radiology can be divided into 4 main subgroups:
1. Vascular Intervention (Arterial) – procedures involving the arteries throughout the body such as angioplasty (balloon dilatation of narrowed blood vessels) or embolisation (blocking off blood vessels to tumours or when someone is bleeding internally).
2. Vascular Intervention (Venous) – procedures involving the veins such as inserting lines into veins, inserting filters to prevent clot travelling around the body (IVC filters) or using devices to suck clot out of blocked veins (thrombectomy).
3. Non-vascular Intervention – procedures not involving the blood vessels such as unblocking kidneys (nephrostomy) or the liver (PTC), injecting cement into collapsed bones (vertebroplasty) or inserting feeding tubes into the stomach (RIG).
4. Interventional Oncology – procedures performed for the diagnosis or treatment of cancer such as tumour ablation (killing tumour cells by inserting a needle into a tumour and heating it up) or injecting chemotherapy coated beads into tumours to kill them (TACE).
Benefits of IR include:
- Reduced physical trauma,
- Reduced pain
- Shorter recovery time
- Less time spent in hospital
- Avoidance of general anesthetics.
IR uses include:
- Treating uterine fibroids
- Opening blocked arteries
- Stroke thrombectomy
- Hemorrhage control
- Venous access for chemotherapy
- Interventional oncology surgery for solid tumors
IR has its own subspecialist areas including interventional neuroradiology and interventional oncology.
Interventional Radiologists must develop skills in:
- Image interpretation
- Patient consultation
- Peri-procedural management
- Procedural performance
Other Specialist Areas
Neuroradiology
Neuroradiologists, steeped in the study of the brain, spine, head, and neck, use imaging technology to diagnose related conditions. Critical skills include:
- Detailed knowledge of neuroanatomy
- Proficiency in neuroimaging technique interpretation
- Understanding associated clinical conditions
Paediatric radiology
Paediatric radiology uses imaging to diagnose and treat conditions in children. X-rays, Ultrasound, Computed tomography (CT) scans, Magnetic resonance imaging (MRI) scans, and Nuclear medicine are all used.
Critical Skills include:
- Selection of the best imaging techniques to diagnose medical and surgical problems in children whose developing bodies are more susceptible to the adverse effects of radiation than adults of equivalent size
- Knowledge of paediatric medicine
- Proficiency in interpretation of radiological examinations in small children
Musculoskeletal (MSK) Radiology
Musculoskeletal (MSK) radiology focuses on diagnosing and treating injuries and diseases of the bones, joints, muscles, and spine. MSK radiologists use X-rays, CT scans, fluoroscopy and ultrasound to perform procedures and interpret images.
What MSK radiologists do:
- Order and interpret medical images of bones, joints, and soft tissues
- Perform image-guided procedures
- Diagnose and treat diseases and injuries of the musculoskeletal system
- Provide imaging guidance during certain procedures
Vascular Radiology
A branch of interventional radiology, vascular radiology, uses imaging to diagnose and treat conditions of the blood vessels and lymphatic system.
How it works
- Uses imaging guidance, such as X-ray, ultrasound, CT scan, or MRI
- Performs minimally invasive procedures, such as stenting, angioplasty, or embolisation
- Uses thin tubes (catheters) and small tools to access blood vessels
Common procedures
- Angiography: An X-ray of the arteries and veins to look for blockages
- Angioplasty: A balloon-tipped catheter is used to open blockages in blood vessels
- Embolisation: A substance is used to stop blood flow through a blood vessel
- Biopsies: A small needle is used to take tissue samples
- Stent placement: A tiny mesh coil is placed in a blood vessel to open a blockage
Head and neck Radiology
Sometimes considered part of Neuroradiology, Head and Neck radiology is an increasingly independent discipline which focuses on the scanning and diagnosis of problems in the head and neck, whether muscular, skeletal, or otherwise. A number of conditions may require head and neck imaging, particularly those related to the Ear, Nose and Throat [ENT].
Gastrointestinal Radiology
Gastrointestinal (GI) radiology uses imaging to diagnose and treat conditions affecting the digestive tract. This includes the stomach, intestines, liver, pancreas, and biliary tree. It uses a variety of imaging techniques, including X-rays, CT scans, ultrasounds, and fluoroscopy. Barium-based contrast materials are often used to help make the GI tract more visible.
Clinical Uses:
GI radiology can help diagnose conditions such as:
- Acid reflux
- Blood in the stool
- Tumors
- Ulcers
- Hernias
- Polyps
- Strictures
- Diverticula
- Inflammation
- Swallowing difficulties
Other GI imaging tests
- An abdominal X-ray can help diagnose causes of abdominal pain, such as masses, blockages, or kidney stones
- A fluoroscopy can take video images of the organs in action
Genitourinary Radiology
Genitourinary (GU) radiology uses imaging to diagnose and treat conditions of the urinary and reproductive systems.
Imaging methods
- X-ray: Uses contrast agents to highlight the urinary system
- Computed tomography (CT): Often the preferred imaging method for emergent conditions
- Ultrasound: Used less frequently than CT for emergent conditions
- Magnetic resonance imaging (MRI): Used to characterize soft tissues
Oncology Radiology
Oncology radiology uses radiation and imaging to diagnose and treat cancer. It involves radiation oncologists, who are physicians who use radiation to treat cancer, and radiologists, who use imaging to diagnose cancer.
How it works
- Imaging - Radiologists use medical imaging, CT scans, MRIs, and X-rays to diagnose cancer.
- Radiation therapy - Radiation oncologists use radiation to treat cancer by damaging the DNA of cancer cells, preventing them from growing and dividing.
- Treatment - Radiation oncologists use the images taken by radiologists to determine the type and amount of radiation to use. They may use radiation alone or in combination with surgery or chemotherapy.
Cardiac Radiology
Cardiac radiology uses imaging to diagnose and treat heart conditions. Cardiac radiologists use a variety of imaging techniques, including X-rays, CT scans, MRIs, and ultrasounds to screen for heart disease, determine the cause of symptoms, monitor the heart, assess the effectiveness of treatments and diagnose structural and functional cardiac conditions.
Cardiac imaging techniques:
- Chest X-ray: A standard imaging technique
- Cardiac MRI: Uses magnetic fields and radio waves to create high-resolution images
- CT scan: A detailed X-ray of the heart and blood vessels
- Echocardiogram: An ultrasound that provides images of the heart
- Nuclear cardiac stress testing: A type of cardiac imaging test
The European Board of Cardiovascular Radiology (EBCR) offers a diploma which helps standardise training and expertise in cardiovascular radiology.
Chest Radiology
Chest radiology uses X-rays to examine the chest and nearby structures. Chest X-rays are the most common radiology exam used to
- assess the condition of lungs and diagnose infection, cancer, or pneumothorax
- assess the size and shape of the heart
- diagnose blood vessel disorders, such as aneurysms
- diagnose calcium deposits in the heart or blood vessels
- assess fractures in the ribs or spine
- detect the presence of a pacemaker, defibrillator, or catheter
Breast Radiology
Breast radiology uses imaging techniques to examine the breasts for screening or diagnostic purposes.
Breast imaging techniques:
- Mammography: A breast X-ray which uses low-energy X-rays to image the breast
- Breast ultrasound: Uses sound waves to create an image of the breast
- Breast magnetic resonance imaging (MRI): Uses magnetic fields to create an image of the breast
Breast radiology uses
- Screening: Mammography can be used to detect breast cancer before symptoms appear
- Diagnosis: Mammography, ultrasound, and MRI can be used to help diagnose breast cancer
Radionuclide radiology
Radionuclide radiology (RNR) comprises those diagnostic imaging techniques which use radio labelled tracers for diagnosis. This includes molecular imaging which provides images of metabolic and physiological processes at the molecular and cellular level. RNR requires an understanding of the physiology and metabolism of radioactive tracers within the body in conjunction with knowledge of normal and pathological anatomy to diagnose the causes of disease and monitor disease progression.
Building Connections with Radiology Subspecialties
A knowledge of radiology specialist fields is important for Resident Medical Officers (RMO) taking their first steps into a career in radiology and applying for training positions. For some potential radiologists, areas of previous clinical practice may be influential in determining specialist interests. For example residents with orthopaedic surgery experience may favour musculoskeletal radiology whilst those with general medical experience may develop interests in chest or cardiac radiology.
With this guide, we hope to empower you in your selection of career interests. If you have more questions or need further assistance, do not hesitate to contact us.
Job Search: view and apply for advertised jobs
Register: Upload your CV and set up job alerts in your chosen area of radiology and location
11 February 2025
Share this post on Social Media